Introduction
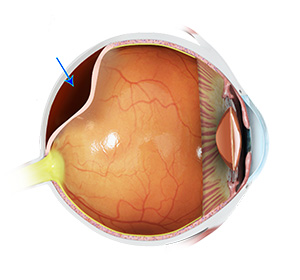
Posterior vitreous detachment (PVD) occurs when the vitreous — the clear, gel-like substance filling the back of the eye — naturally shrinks and separates from the retina. This is a common age-related change and is usually harmless, but in some cases, it can lead to complications if the retina is pulled or torn during the process.
While PVD itself often doesn’t require treatment, it can cause symptoms such as floaters or flashes of light that should be promptly assessed to rule out retinal tears or detachment. Early evaluation by an eye specialist is important to protect vision and manage any associated risks.
Causes and Risk Factors of Posterior Vitreous Detachment
What Causes Posterior Vitreous Detachment?
Posterior vitreous detachment is usually a natural part of aging, but certain factors can increase the likelihood of it occurring earlier or leading to complications. Knowing the causes and risk factors can help you recognise symptoms and seek timely evaluation.
Common causes and risk factors include:
- Age-related changes
The vitreous gel naturally shrinks and becomes more liquid with age, leading to separation from the retina. - Nearsightedness (myopia)
People with longer eyeballs are more likely to develop PVD at a younger age. - Eye trauma
Injury to the eye can trigger vitreous separation. - Previous eye surgery
Procedures like cataract surgery can increase the risk of PVD. - Inflammation inside the eye
Conditions that cause intraocular inflammation can speed up vitreous changes. - Retinal disorders
A history of retinal tears or detachments may make the vitreous more prone to separating.
Recognising these factors can help you take early action if symptoms appear, reducing the risk of serious retinal complications.
Types of Posterior Vitreous Detachment
The Different Types of Posterior Vitreous Detachment
PVD can vary in how it develops and whether it is accompanied by complications. Understanding the type helps guide monitoring and treatment.
Complete PVD
- Description:
The vitreous gel has fully separated from the retina and optic nerve head. - Who it affects:
Most common in older adults, typically over age 60. - Speed of progression:
Usually develops gradually over weeks or months.
Partial PVD
- Description:
The vitreous has detached from part of the retina but remains attached in other areas. - Who it affects:
Can occur at any age but more frequent in those with myopia or after eye surgery. - Speed of progression:
May progress slowly to complete PVD or remain stable for years.
PVD with Vitreomacular Adhesion (VMA)
- Description:
The vitreous remains tightly attached to the macula (central retina), which can cause visual distortion or macular damage. - Who it affects:
More likely in people with high myopia, diabetes, or retinal conditions. - Speed of progression:
Can be stable or progress quickly, potentially leading to macular hole formation.
Complicated PVD
- Description:
PVD that leads to retinal tears, retinal detachment, or vitreous haemorrhage. - Who it affects:
Those with a history of retinal problems, trauma, or inflammatory eye disease. - Speed of progression:
May occur suddenly and requires urgent treatment.
Early Signs & Symptoms
Common Symptoms of Posterior Vitreous Detachment
Recognising the signs of PVD early helps ensure prompt assessment and detection of possible complications like retinal tears or detachment.
- Floaters in vision
Small dark specks, threads, or cobweb-like shapes drifting across your sight. - Flashes of light (photopsia)
Brief bursts of light, often more noticeable in dim lighting or when moving the eyes. - Blurry or hazy vision
Vision may become less clear, especially in the early stages of detachment. - Shadow or curtain in vision (urgent sign)
May indicate a retinal tear or detachment and needs immediate medical attention. - Sudden increase in floaters or flashes
A rapid change in symptoms may signal a complication requiring urgent care.
Diagnosis and Treatment of Uveitis and Ocular Inflammation
Posterior vitreous detachment is diagnosed through a comprehensive eye examination, including dilated fundoscopy to assess the vitreous and retina. Optical coherence tomography (OCT) may also be used to get detailed images of the retina’s structure. While PVD itself is usually harmless and does not require treatment, close monitoring is essential to detect any complications like retinal tears or detachments early. If such complications occur, prompt surgical intervention may be necessary to prevent vision loss.
Why Timely Diagnosis Matters
Early diagnosis of posterior vitreous detachment is important to monitor for potential complications such as retinal tears or detachment, which can threaten vision if left untreated. Prompt assessment ensures timely intervention to prevent serious damage and preserve sight.
Timely diagnosis allows your ophthalmologist to:
- Confirm the presence of PVD and differentiate it from more serious retinal conditions
- Monitor the vitreous and retina for any signs of tears or detachment
- Provide early treatment if complications arise to avoid permanent vision loss
- Educate you on warning signs to watch for and when to seek immediate care
- Help maintain overall eye health and visual function
Addressing posterior vitreous detachment early helps ensure the best possible outcomes and protects your vision.
Continue Learning About Other Eye Conditions
Other Eye Conditions
The eyes are the most complex sensory organ in our bodies. The eyes provide vision by recording images of our surroundings that the brain will interpret. Although the eye measures only about an inch...
Proliferative Diabetic Retinopathy
Diabetic retinopathy is a complication of diabetes, characterised by progressive damage to the retina. The condition usually affects both eyes and the severity can vary...
Worried About Your Vision?
Schedule a consultation with Mr. Mo Majid to evaluate your eye health.
Quick Answers About Posterior Vitreous Detachment
What is posterior vitreous detachment (PVD)?
PVD occurs when the gel-like vitreous inside the eye shrinks and pulls away from the retina, which is a natural part of aging.
What symptoms should I watch for with PVD?
Common signs include sudden flashes of light, new floaters, or cobweb-like shadows in your vision.
Is PVD dangerous?
While PVD itself is usually harmless, it can sometimes cause retinal tears or detachment, which require urgent treatment to prevent vision loss.